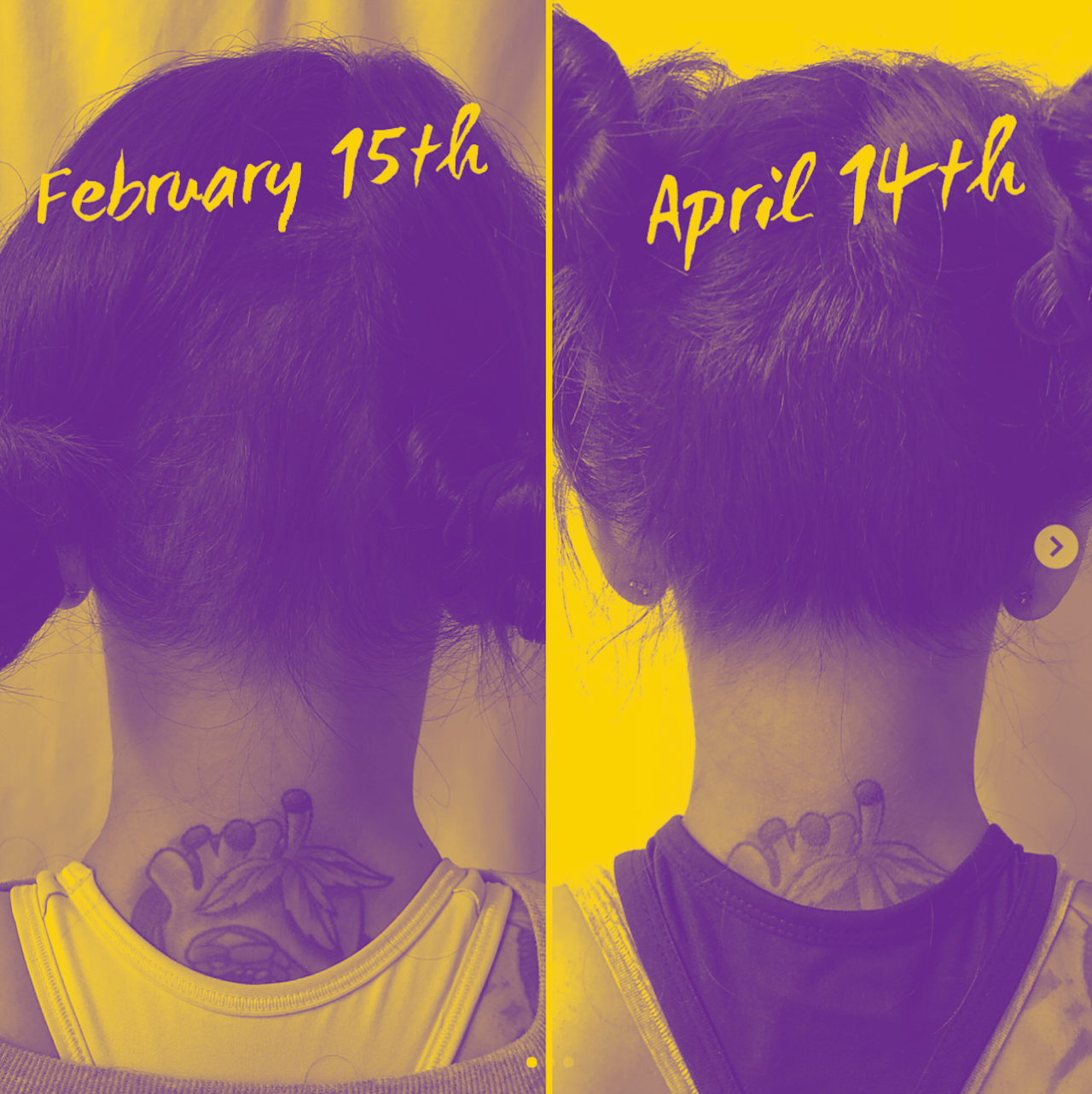For anyone diagnosed with cancer the biggest fear (aside from the obvious) is the prospect of chemotherapy. The word “chemo” conjures up our worst, most visceral mental images of a cancer patient — someone who is thin, bald, sick. When I was diagnosed with breast cancer earlier this year, the prospect of months of gruelling chemotherapy left me near-paralyzed with fear.
Chemotherapy is a type of cancer treatment that attacks all rapidly dividing cells in your body. Cancer is, by its very nature, the rapid division of cells, so chemo can stop cancer in its tracks. Unfortunately, the other type of rapidly dividing cell in your body is the hair follicle, which means chemotherapy, particularly the variety used to treat breast cancer, almost always results in total hair loss. While I didn’t want to spend six months bedridden and vomiting, with my immune system destroyed, worried that the poisons I was willingly pumping through my veins wouldn’t succeed in obliterating the tumor trying to kill me, I also worried about how I’d be seen by the rest of the world. I didn’t want to be a sick person, and I didn’t want cancer to subsume my identity.
Prior to entering the “cancer world,” I had no idea a process called cold capping existed. But when a nurse told me it might help me keep my hair, I could have kissed her. It was, among the endless barrage of bad news, something to feel good about. I decided right then to do it.
A cold cap is exactly what it sounds like: a helmet worn during chemotherapy that, using dry ice or frozen gel, lowers the temperature of the scalp and forces hair follicles to “sleep.” When the follicles are dormant, they’re not dividing, and therefore chemotherapy drugs don’t attack them. In theory, cold capping prevents hair loss and allows for better regrowth after chemotherapy ends.
Scalp cooling can be painful and the results of it are variable, but fundamentally, it does what it’s supposed to do — it retains hair.
I finish chemotherapy this week. After eight infusions and 24 weeks, my hair has thinned, but not noticeably so. If you met me, you probably wouldn’t know I have cancer. Scalp cooling can be painful and the results of it are variable, but fundamentally, it does what it’s supposed to do — it retains hair.
But it’s also so much more than that. Whether the results of cold capping are good or bad, it gives women like myself an element of control over their treatment at a time when everything their life is out of their control. It is, quite literally, changing the face of modern cancer.
I used Paxman-brand cold cap, a machine-based cold-cap system which was provided for free under the National Health Service, partially because it was free, and partially because, as a regulated machine, I could rely on nurses at hospital to operate it for me, eliminating the stress of having to do it myself. Originally a family business that patented its own beer-cooling system used in breweries across the UK, Paxman entered the world of cold capping when its founder, Eric Paxman, saw his daughter-in-law lose her hair while undergoing chemotherapy for breast cancer. Eric’s son Glenn then adapted the family’s cooling system to develop the first prototype of the Paxman cold cap, which debuted in 1997.
Nowadays, Paxman caps are available at 95 percent of hospitals in Britain and 130 hospitals across the U.S. The company is overseen by Richard Paxman, Eric’s grandson, who was deeply affected by his mother’s breast-cancer journey. “What we do is so important to me and to my mum’s legacy,” Richard told The Outline. “And we’re working so hard to make scalp cooling available to all of those who want to use it, not just to those who can afford it.” Paxman currently works with HairToStay, a San Francisco-based charity founded to help support patients whose health insurance does not cover cold capping. Despite this, however, Richard said that scalp cooling remains a relatively obscure treatment.
“Sadly, not enough people know about scalp cooling,” he said. “We’re working hard to increase awareness but it’s difficult.”
Physically, scalp cooling is extremely painful. My regimen meant that each of my chemotherapy sessions were 90 minutes to two-and-a-half hours longer than average, meaning for some days I was at hospital for up to eight hours at a time; it’s necessary to wear the cold cap while chemotherapy drugs are flowing into your system and the machine takes half an hour to freeze and then warm up again. For some patients, the day can be even longer, especially for those who choose to do manual caps with dry ice A patient only needs to cold cap on the days they’re undergoing chemotherapy, but that one day every two or three weeks can be incredibly tiring. Even after chemotherapy is over, hair continues to shed for several weeks until the drugs and their side effects finally leave your system.
Unless I decided to tell people, nobody knew I was sick... my surgeon was shocked by my decidedly hairy appearance.
But the technology is, for anyone faced with the prospect of losing their hair, nothing short of remarkable. I underwent 24 weeks of ACT chemotherapy, which is well known for complete hair-loss without cold-capping. While I experienced thinning throughout, especially during my weekly hairwashes, I estimate that I kept 70 to 80 percent of my hair overall. Unless I decided to tell people, nobody knew I was sick, and when I was admitted to hospital to have my surgery after chemotherapy ended my surgeon was shocked by my decidedly hairy appearance. So why isn’t cold-capping more widespread?
Because of the variable results and the extreme pain and discomfort scalp-cooling can cause, cold-capping tends to be dismissed by doctors. This attitude seems to stem partially from cold-capping still being seen as “experimental” and partially because of the backseat “cosmetic” concerns like going bald take for doctors who, of course, are just there to make sure cancer doesn’t kill you. Though it received FDA approval in 2017, citing a study that showed 66 percent of patients who cold-capped lost less than half of their hair, the practice is typically not fully covered by insurance (though certain plans cover wigs for cancer patients, which can cost thousands of dollars). As a result, cold capping proponents have formed a community online to support each other. “I felt so hopeless when it came to knowledge on capping and I didn’t want to accept that,” said Becca Jean Munoz, who founded the 500-member strong Chemo Cold Cappers Support Group on Facebook, said. “There is so much information on cancer as a disease on blogs, message boards, forums and groups but a lot of dead ends when it comes to information on capping.”
Becca was just 29 when, in summer of 2017, she felt the lump that would change her life forever. By the time she was diagnosed her breast cancer had already progressed to stage two, requiring a mastectomy and months of chemotherapy. Like many young people fighting cancer, Becca, who lives in Austin, Texas, wanted her life to remain as normal as possible, and that meant not looking like a “sick person.”
“The thought of having a chance to save my hair and keep my life as close as possible to what it was before diagnosis was and is still very important to me,” she said. But she initially faced resistance and negativity over the efficacy of cold caps from her medical team. “One chemo tech scoffed at me and said ‘sweetie, they don’t work.’”
Becca had to travel to San Antonio for her cold capping treatment, and each session cost $500. “I absolutely believe cold capping should be covered with insurance,” she told me. “Hair is seen as strictly a beauty issue, but it serves a function too. It protects us from UV exposure and regulate[s] our temperature.” During chemotherapy, skin is more sensitive and can burn easily under UV exposure; even a slightly elevated or decreased temperature can result in sepsis, which for anyone with an impaired immune system can be fatal. “It’s frustrating that it’s treated as a cosmetic issue. Insurance codes are yet to catch up with cancer technology,” she added. Becca, who was a student at the University of Texas at the time of her diagnosis, is now dedicating herself to helping cold cappers and cancer patients full-time.
Emily Boullet, a young mother from Oregon who was diagnosed with breast cancer in 2017, wanted to keep her hair so her young daughters wouldn’t be upset by her appearance. Emily chose a manual cold-capping system, which meant changing her own dry-ice caps frequently. Like Becca, she faced problems with her insurance company.
“My insurance company offered me $2,500 for a wig, but nothing to cover the capping,” Boullet said. “The dry ice each time was around $70 (for 16 chemotherapy infusions), and the rental of the caps themselves was $500 a month. I do think more people would know about and use cold caps if they had the support of their insurance companies.”
Along with the cost of cold capping, the regime can be punishing. After chemotherapy sessions, those who cold cap must keep their scalps from getting hot — which means washing their hair in cold water no more than once a week and not using a hair dryer. Dyeing hair is out, as is cutting it, as this can supposedly “shock” the follicle used to the current weight and length of your hair and cause it to fall out. Despite abiding by these particularities, Boullet still lost 90 percent of her hair.
“I went into this with the expectation that I’d be able to camouflage my chemo treatments, but I was one of the unlucky ones who lost nearly everything,” Boullet said. “There were several nights I would sob and be ready to shave everything off, but I persevered in the hope that cold-capping would help me with regrowth. I’m now nine weeks out of chemo and already have a full head of hair again, ready for a trim.” While the results were disappointing for Boullet, she still achieved the simple thing that many cancer patients hope for — the ability to mentally move on from cancer after finishing chemo because they don’t still “look sick.”
The practice is also slowly becoming more visible in the media. Shannen Doherty, who was diagnosed with breast cancer in 2015, is among the few who have spoken publicly about her experience with the process, posting a photo of herself during chemotherapy, in October last year to coincide with Breast Cancer Awareness month. Some outlets speculated that Julia Louis Dreyfus also underwent cold capping while going through chemotherapy for breast cancer in late 2017. When an episode of Jane The Virgin earlier this year depicted cold-capping during chemotherapy for breast cancer, it was a TV first.
“I can see myself crossing the finish line,” the character Xo tells her husband Rogelio in the episode. “Which is why I’ve decided to do those cold caps. I’ll feel so much better if I can finish chemo with my hair. Get on with my life and leave cancer behind me.”